Everyday there is something interesting I learn about Johne’s disease and it comes from diverse sources. This story is about –
comparative pathology
and
collaborative learning
The email below was received last week from Dr. Fritz Schumann, a Canadian veterinarian working in Saskatoon (see map):
He wrote: I am vet in Saskatoon. I had this 2 year and 9-month-old Black Angus cow which I euthanized as she had Johne’s. Positive ELISA in blood and PCR positive on feces. I euthanized her and am sending two pictures. The first is her ileum and jejunum. The second picture is the aorta, looks like calcification from the aortic valve all the way to the pelvis then I stopped looking. The aorta felt like there is no elastic tissue left and paper thin. My question is why does aorta change like that with Johne’s? This is the worst aorta I have seen. Thank you very much for reading my email and considering my request for an explanation.
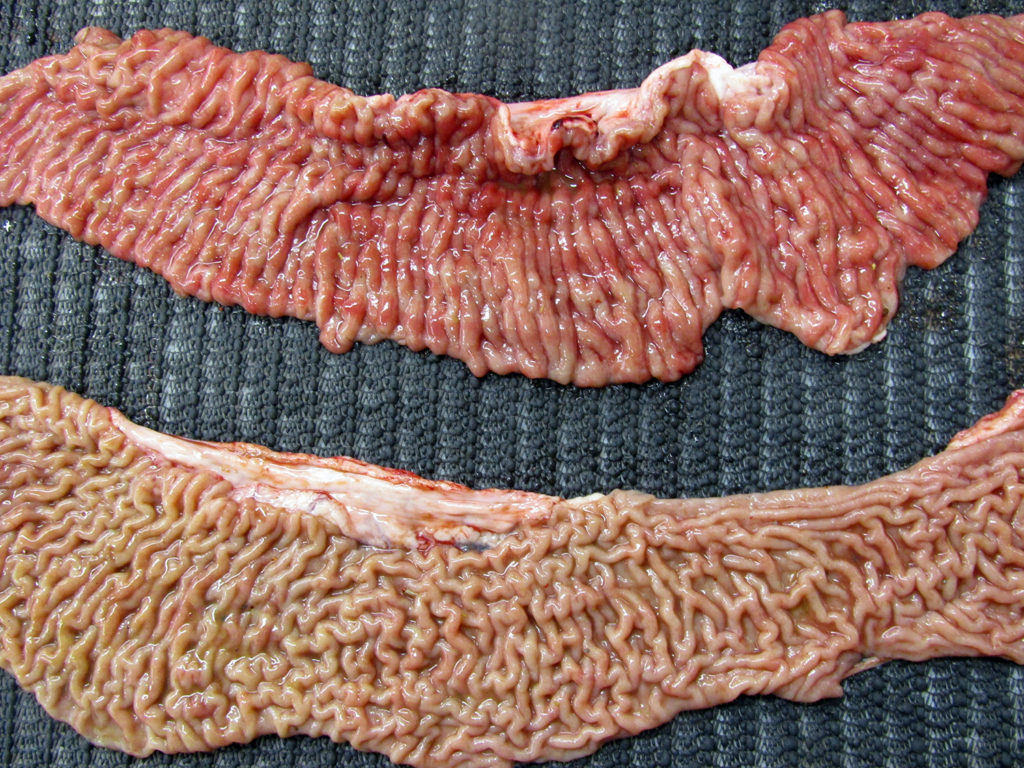
THANK YOU DR. SCHUMANN! He granted me permission to show his exceptional pictures taken at the Western College of Veterinary Medicine. The first shows the classic thickened ileum (top) and the jejunum for comparison (bottom).
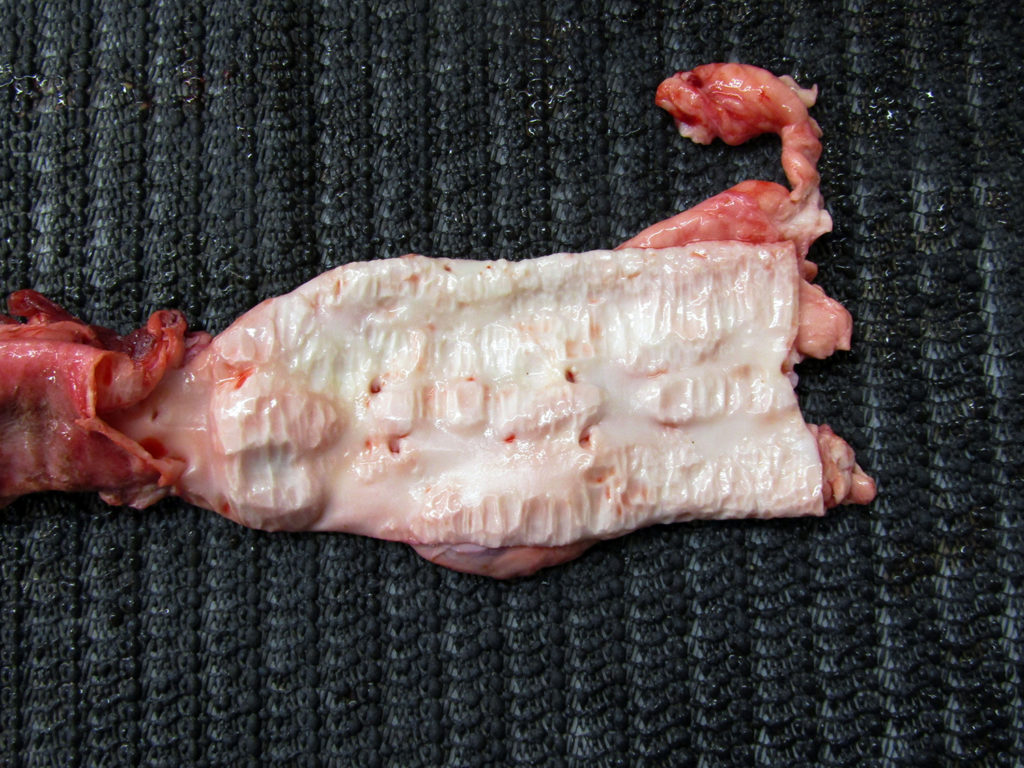
This second photo shows the striking degree of calcification of the aorta.
I made inquiries with colleagues and this reply came from the Minnesota Veterinary Diagnostic Laboratory pathologists. Below is their quick and informative reply. Big thanks! to these pathologists.
Provided here is an excerpt from a paper that was published in JVDI on blastomycosis in a llama (J Vet Diagn Invest. 2018 Jul; 30(4): 576–579). It provides some thoughts on possible pathogenesis:
“As a component of chronic disease, monocytes and macrophages can generate and release tumor necrosis factor–alpha (TNFα) that drives mineralization, and macrophages may accumulate basic calcium phosphate that can locally increase cytokine production (TNFα, interleukin [IL]-1, and IL-8) that further drives mineralization and stimulates endothelial cells to differentiate toward osteoblasts (20). In dromedary camelids and cattle with Johne’s disease, which exhibits a predominantly granulomatous cellular response, proinflammatory cytokines (IL-1α, IL-1β, IL-6, IL-10, interferon-γ, and TNF-α), acute-phase and oxidative-stress proteins are significantly increased (9). Hypercalcemia has been reported in dogs with granulomatous diseases, including blastomycosis, and is likely associated with the conversion of calcifediol (25-hydroxyvitamin D) to calcitriol (1,25-dihydroxyvitamin D) by activated macrophages (8,14).”
Citations mentioned in this 2018 JVDI excerpt:
- #8. Dow SW, et al. Hypercalcemia associated with blastomycosis in dogs. J Am Vet Med Assoc 1986;188:706–709.
- #9. El-Deeb W, et al. Clinico-biochemical investigation of paratuberculosis of dromedary camels in Saudi Arabia: proinflammatory cytokines, acute phase proteins and oxidative stress biomarkers. Pak Vet J 2014:34;484–488.
- #14. Meuten D. Parathyroid glands and calcium and phosphorus metabolic pathology. In: Thrall MA, et al., eds. Veterinary Hematology and Clinical Chemistry. 2nd ed. Ames, IA: WileyBlackwell, 2012:545–568.
- #20. Shantsila E, Lip GY. Systemic inflammation as a driver of vascular calcification: a proof of concept. J Intern Med 2009;266:453–456.
I am also providing a link to the excellent 1978 article by Dr. Claus Buergelt and colleagues on the pathology of bovine paratuberculosis which mentions aortic calcification.
______________
Comment: This report is a perfect example of how an inquisitive veterinary practitioner requested a necropsy on a cow with Johne’s disease, how veterinary pathologists documented some novel pathology, how the practitioner reached out via the internet to learn more, and how personal and internet connections helped everyone reading this post to know more about the pathobiology of Johne’s disease. In many ways it mirrors the how the first report of Johne’s disease came to be.
______________
And…..for the keenly interested, here are some additional related references with links. This is not an exhaustive list. Sorry if I missed your favorite publication:
- US Sorge et al. Cow-level association between serum 25-hydroxyvitamin D concentration and Mycobacterium avium subspecies paratuberculosis antibody seropositivity: A pilot study. Journal of Dairy Science. 96(2):1030-1037, 2013.
- JR Stabel et al. Dietary calcium modulates Mycobacterium paratuberculosis infection in beige mice. Veterinary Immunology and Immunopathology, 66(3–4): 377-390, 1998.
- RW Jayalath et al. Aortic calcification. European Journal of Vascular and Endovascular Surgery. 30(5):476-488, 2005.
- N Niederhoffer et al. Aortic calcification produced by vitamin D3 plus nicotine. Journal of Vascular Research. 34(5):386-398. 1997.